Recognising the tremendous pressure that health, VCSE and local authority leaders are under as a result of the Covid-19 outbreak, IVAR and SEUK are facilitating online peer support groups through their Practice Development Network[i] (PDN), which supports cross-sector partnership working in healthcare settings. The aim is to create a space for people to share experience thoughts and learning, during the pandemic at a time of pressure on the health system for those working navigating and delivering in partnership.
We find them a fascinating snapshot of hope and perseverance, and it is brilliant to see connections being made in real time that can help unblock a challenging situation, in another region.
We were joined by 20 cross-sector health and care leaders on 21st May for our two virtual peer support sessions. They were from different parts of England including: Bedfordshire, Luton and Milton Keynes; Dorset; Surrey Heartlands, Northamptonshire; Worcestershire; Liverpool; Leeds; Stoke-on-Trent; Nottinghamshire; Lancashire and South Cumbria; Northumberland; and London.
Building trust rapidly
It was interesting to hear the positive stories that people shared about the speed and flexibility in their processes to re-designed or developed their services to cope with the new way of working for their varied service users. For example, a mental health support service is now being run digitally and is having more interaction with people than before when it was a drop-in, face-to-face service. Not only had this made a huge difference to many people, in some cases preventing suicide, it also offers solutions to those in rural areas facing transport issues. ‘People tend to enjoy a bit more anonymity on the call, especially those we have less motivation to physically take themselves to the clinic.’
Key to this was a change in focus from box checking governance to pursuing relationships based on trust, and an assumption by all partners that people would do the ‘right thing’. This was something that all wanted to hold onto, to sustain as areas began to look at their priorities for starting up services that had been suspended to cope with Covid-19.
‘There is a massive desire amongst a few of us to keep pushing cross-sector working.’
‘We need to take time to pause and reflect, the good stuff that is going on and plan to continue this in the future.’
Long term versus short term
This is where discussion turned to barriers in cross-sector working and how to support systems’ need to see past immediate priorities – of catching up with waiting lists – and not ignoring equally important projects that seek to address longer-term issues through community resilience. This is the paradox that for some areas the experience of the last two to three months have made this incredibly easy, and convinced leaders within their ICS or system that prioritising community resilience and supporting the VCSE to be an equal partner in this is key, while others have drawn up the metaphorical drawbridge and have even less time and money for approaches of this kind.
It is often about the art of the possible, and perhaps this is where sharing experiences and learning is even more important, if people can see others taking a different approach, it can lead to adopting different ways of working.
Using data to embed social prescribing and tackle health inequalities
This was further emphasized by a case study in North Dorset, shared by Dr Simone Yule. She leads on Population Health Management (PHM)[ii] for the ICS. North Dorset previously received support from NHS England and Improvement to develop their PHM skills and data. Dr Yule shared how they were using this approach to managing data to ensure those most in need during the pandemic were getting the support that they needed. Being able to search their Practice data for people with a number of underlying health conditions that might make them more vulnerable to Covid-19, and were then able to link them up with appropriate support either via a health champion or social prescriber. See matrix below for intervention.
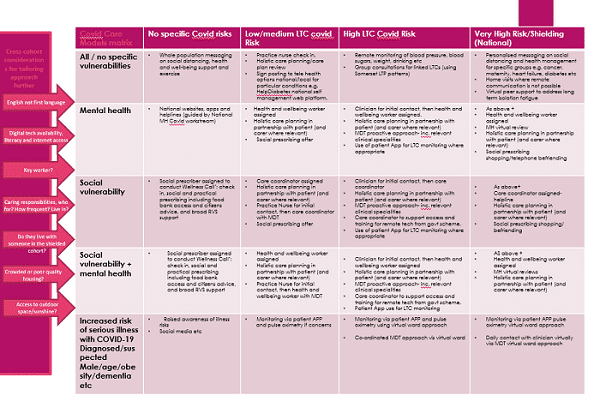
Data sharing
Many people on the call were keen to understand the approach to data sharing, since this has been a barrier for many to develop a comprehensive and embedded approach to social prescribing in primary healthcare. It had also hampered people’s ability to respond in the current pandemic, with CCGs being unwilling to share shielding data with the VCSE due to existing data sharing agreements. From Dr Yules’ perspective, their CCG had been very supportive, waiving some governance control to ensure the right people were supported in a timely manner, letting link workers know that they were trusted to do the right thing. Even though some patients had withdrawn consent to be contacted, the emergency situation allowed the Practice to override this request and all at risk patients had been contacted. There have been no complaints.
Enabling transformation
Returning to the theme throughout the discussion, many were nervous that things would return to pre-pandemic ways, with a focus on governance and reporting outputs and counting interactions which would not support an ongoing transformation of care and support within the healthcare system. As the last few months have demonstrated, relaxing governance and trusting organisations and individuals to do the right thing has enormous benefits and can support radical and rapid change for the better. We need to ensure that this can be adopted in a sustainable way to drive forward the positive benefits seen in the collective response to Covid-19.
Resources
Resources for building cross-sector relationships that improve community-based healthcare can be viewed and downloaded from here.
[i] Practice Development Network (PDN): The PDN is designed to support the sharing of learning, experiences and challenges of working in a collaborative way across sectors in health and social care. Its core members are people who have been involved in Building Health Partnerships and Transforming Healthcare Together, however it is open to all who are working or would like to work across sectors to deliver better health and social care outcomes. The network consists of an email group, allowing individuals to share helpful resources and make useful connections between each other as well as regular webinars. To join the email group email: Nancy.towers@socialenterprise.org.uk
[ii] Population Health Management is an emerging technique for local health and care partnerships to use data to design new models of proactive care and deliver improvements in health and wellbeing which make best use of the collective resources.
